Availity Prior Authorization Form
Availity Prior Authorization Form - Web the availity provider portal is now humana’s preferred method for medical and behavioral health providers to check eligibility and benefits, submit referrals and authorizations, manage claims and complete other secure administrative tasks online. Complete a short questionnaire, if asked, to give us more clinical information. Checks service codes against a payer database, providing confirmation and reducing calls and unnecessary paperwork. Please complete this form \(step 1\), have it notarized \(step 2\), and return the original notarized \. Available through the availity essentials or intelligent gateway. Web eligibility and benefits prior authorization and status claims and payments electronic funds transfer (eft) includes enrollment and cancellation get a head start and begin using availity now so that your office staff is up to speed on all things availity by september 10. Review and submit your request. Web to obtain access to availity essentials, availity, llc, requires that users verify their identity manually when electronic verification is unsuccessful. Select patient registration menu option, choose authorizations & referrals, then authorizations. Select a request type and start request.
Submit your initial request on availity with the authorization (precertification) add transaction. Complete a short questionnaire, if asked, to give us more clinical information. Select patient registration menu option, choose authorizations & referrals, then authorizations. Frequently asked questions about the transition. Allows providers to check to see if an authorization is required before initiating a request. It’s ideal for direct data entry, from eligibility to authorizations to filing claims, and getting remittances. Web how to access and use availity authorizations: Select payer bcbsil, then choose your organization. Review and submit your request. Web online, direct data entry with intuitive workflows.
Review and submit your request. Select patient registration menu option, choose authorizations & referrals, then authorizations. Frequently asked questions about the transition. Available through the availity essentials or intelligent gateway. Select a request type and. Please complete this form \(step 1\), have it notarized \(step 2\), and return the original notarized \. Web eligibility and benefits prior authorization and status claims and payments electronic funds transfer (eft) includes enrollment and cancellation get a head start and begin using availity now so that your office staff is up to speed on all things availity by september 10. Complete a short questionnaire, if asked, to give us more clinical information. Web how to access and use availity authorizations: Select patient registration menu option, choose authorizations & referrals, then authorizations *.
Bcbs Prior Authorization Form Pdf Fill Out and Sign Printable PDF
It’s ideal for direct data entry, from eligibility to authorizations to filing claims, and getting remittances. Please complete this form \(step 1\), have it notarized \(step 2\), and return the original notarized \. Available through the availity essentials or intelligent gateway. Submit your initial request on availity with the authorization (precertification) add transaction. Complete a short questionnaire, if asked, to.
Fill Free fillable Availity Providers PDF forms
Visit availity.com/premera to register with availity and get training. Checks service codes against a payer database, providing confirmation and reducing calls and unnecessary paperwork. Please complete this form \(step 1\), have it notarized \(step 2\), and return the original notarized \. Allows providers to check to see if an authorization is required before initiating a request. Select a request type.
FREE 11+ Prior Authorization Forms in PDF MS Word
Please complete this form \(step 1\), have it notarized \(step 2\), and return the original notarized \. Web how to access and use availity authorizations: Allows providers to check to see if an authorization is required before initiating a request. Complete a short questionnaire, if asked, to give us more clinical information. Visit availity.com/premera to register with availity and get.
Universal prior authorization form in Word and Pdf formats
Please complete this form \(step 1\), have it notarized \(step 2\), and return the original notarized \. Select a request type and start request. Select a request type and. Visit availity.com/premera to register with availity and get training. Web the availity provider portal is now humana’s preferred method for medical and behavioral health providers to check eligibility and benefits, submit.
Medicare Generation Rx Prior Authorization Form Form Resume
Visit availity.com/premera to register with availity and get training. Select a request type and start request. Select payer bcbsok, then choose your organization. Select payer bcbsil, then choose your organization. Web to obtain access to availity essentials, availity, llc, requires that users verify their identity manually when electronic verification is unsuccessful.
Authorization Form Fill Out and Sign Printable PDF Template signNow
Please complete this form \(step 1\), have it notarized \(step 2\), and return the original notarized \. Select a request type and start request. Web how to access and use availity authorizations: Select payer bcbsok, then choose your organization. Checks service codes against a payer database, providing confirmation and reducing calls and unnecessary paperwork.
FREE 8+ Sample Prior Authorization Forms in PDF MS Word
Checks service codes against a payer database, providing confirmation and reducing calls and unnecessary paperwork. Select a request type and start request. Visit availity.com/premera to register with availity and get training. It’s ideal for direct data entry, from eligibility to authorizations to filing claims, and getting remittances. Select payer bcbsil, then choose your organization.
New Prior Authorization & Referral Submission Tool via Availity
Select a request type and start request. Web the availity provider portal is now humana’s preferred method for medical and behavioral health providers to check eligibility and benefits, submit referrals and authorizations, manage claims and complete other secure administrative tasks online. Web how to access and use availity authorizations: Frequently asked questions about the transition. Select payer bcbsok, then choose.
Aarp Prior Authorization Form Form Resume Examples dP9lDOk9RD
Allows providers to check to see if an authorization is required before initiating a request. Visit availity.com/premera to register with availity and get training. Web how to access and use availity authorizations: Web how to access and use availity authorizations: Available through the availity essentials or intelligent gateway.
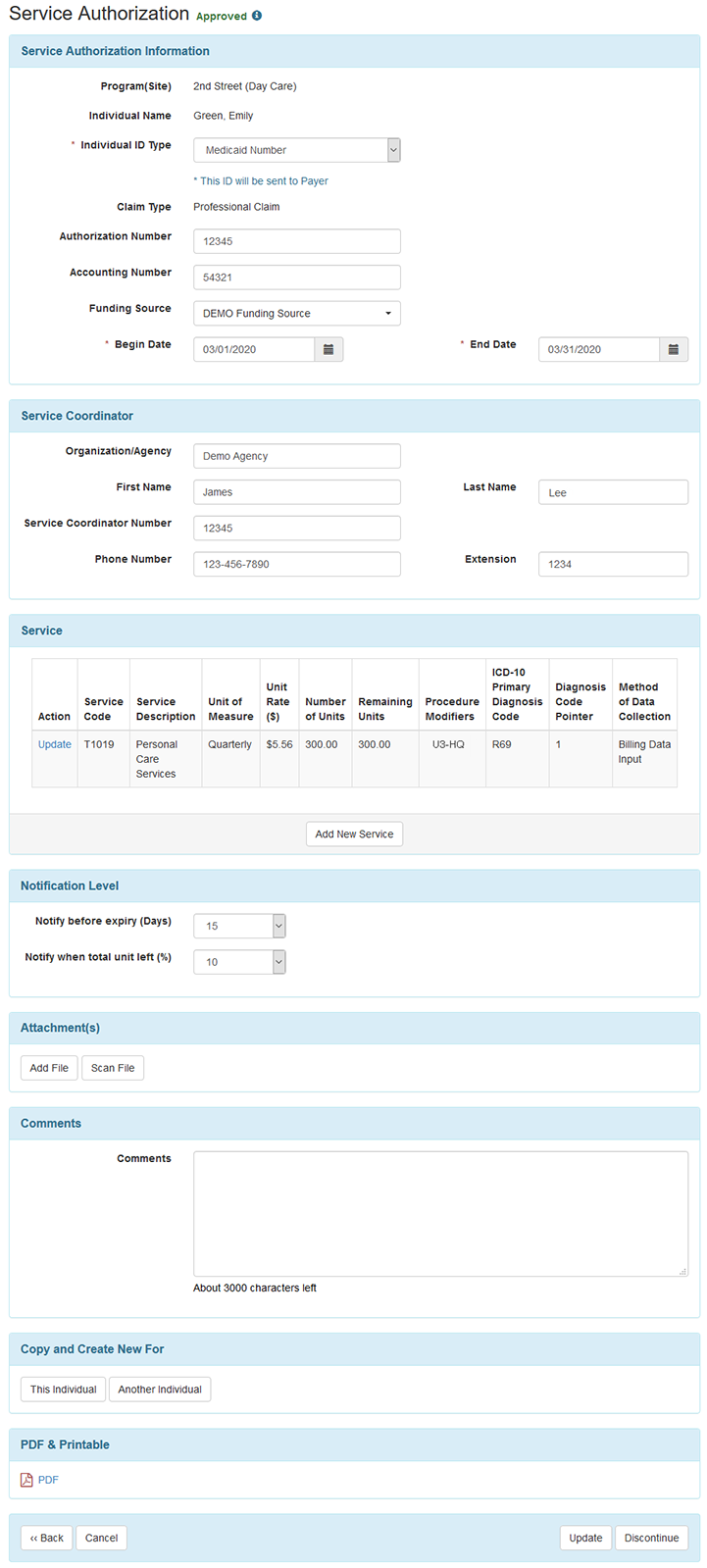
Service Authorization Therap
Select payer bcbsok, then choose your organization. Select a request type and start request. Select a request type and. Select patient registration menu option, choose authorizations & referrals, then authorizations. Complete a short questionnaire, if asked, to give us more clinical information.
Web Online, Direct Data Entry With Intuitive Workflows.
Web eligibility and benefits prior authorization and status claims and payments electronic funds transfer (eft) includes enrollment and cancellation get a head start and begin using availity now so that your office staff is up to speed on all things availity by september 10. Web the availity provider portal is now humana’s preferred method for medical and behavioral health providers to check eligibility and benefits, submit referrals and authorizations, manage claims and complete other secure administrative tasks online. Frequently asked questions about the transition. Please complete this form \(step 1\), have it notarized \(step 2\), and return the original notarized \.
Submit Your Initial Request On Availity With The Authorization (Precertification) Add Transaction.
Select payer bcbsil, then choose your organization. Available through the availity essentials or intelligent gateway. Select patient registration menu option, choose authorizations & referrals, then authorizations. Visit availity.com/premera to register with availity and get training.
Review And Submit Your Request.
It’s ideal for direct data entry, from eligibility to authorizations to filing claims, and getting remittances. Complete a short questionnaire, if asked, to give us more clinical information. Checks service codes against a payer database, providing confirmation and reducing calls and unnecessary paperwork. Allows providers to check to see if an authorization is required before initiating a request.
Select A Request Type And Start Request.
Select payer bcbsok, then choose your organization. Web to obtain access to availity essentials, availity, llc, requires that users verify their identity manually when electronic verification is unsuccessful. Web how to access and use availity authorizations: Select patient registration menu option, choose authorizations & referrals, then authorizations *.